This article provides general educational information only. It does not constitute medical or legal advice, diagnosis, or treatment. Medical conditions, injuries, and insurance matters vary by individual and jurisdiction. Readers should consult licensed medical and legal professionals for guidance specific to their situation.
Concussions After Car Accidents: An Informational Overview
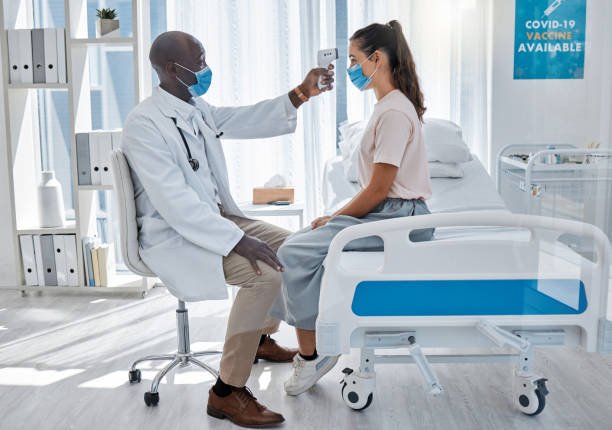
Concussions are among the more frequently reported injuries following motor vehicle collisions. Because they do not always involve visible trauma or immediate symptoms, they may go unrecognized at the scene of an accident or in the hours that follow. This article provides general educational information about concussions related to car accidents, including how they occur, how symptoms may present, and how such injuries are commonly evaluated in medical and insurance contexts.
What Is a Concussion?
A concussion is classified as a form of mild traumatic brain injury (often abbreviated as “mild TBI”). The term “mild” refers to the absence of observable structural damage on standard imaging, such as fractures or intracranial bleeding, rather than the severity of symptoms experienced.
A concussion occurs when rapid movement causes the brain to shift inside the skull. This movement can temporarily disrupt normal brain function, affecting cognition, balance, mood, and sensory processing.
Concussions may occur as a result of:
-
A direct impact to the head
-
An object striking the head
-
Sudden acceleration or deceleration of the body
-
Rapid forward-and-backward movement of the neck
Loss of consciousness is not required for a concussion to occur, and symptoms are not always immediately apparent.
How Concussions Commonly Occur in Car Accidents
During a car accident, forces generated by sudden stops, impacts, or directional changes can cause the brain to move within the skull. This can happen even in collisions that do not involve head contact with another object.
Concussions may occur even in lower-speed collisions, depending on factors such as vehicle position, occupant movement, restraint use, restraint use, and angle of force. Because external signs of injury may be absent, concussions are sometimes identified only after symptoms develop.
Commonly Reported Symptoms
Symptoms associated with concussions can vary in type, severity, and duration. Some individuals report symptoms immediately, while others experience delayed onset hours or days after the incident.
Commonly documented symptoms include:
-
Headache or head pressure
-
Dizziness or balance difficulties
-
Nausea
-
Sensitivity to light or sound
-
Difficulty concentrating
-
Slowed thinking or response time
-
Memory disruption
-
Fatigue
-
Visual disturbances
-
Sleep pattern changes
-
Emotional or mood changes
Not all symptoms are present in every case, and symptom patterns may fluctuate during recovery.
Delayed Symptom Presentation
Delayed symptom onset is widely recognized in concussion research. In the period immediately following an accident, heightened stress responses may temporarily mask symptoms. As inflammatory processes develop, symptoms may become more noticeable.
The timing of symptom appearance alone does not determine injury validity. Medical evaluations often consider the mechanism of injury, symptom progression, and clinical findings together rather than relying on timing in isolation.
How Concussions Are Evaluated Medically
There is no single diagnostic test that definitively confirms a concussion. Instead, medical professionals typically rely on a combination of clinical assessments.
These evaluations may include:
-
Neurological examinations
-
Cognitive and memory assessments
-
Balance and coordination testing
-
Symptom history review
-
Imaging studies when necessary to rule out more serious conditions
Standard imaging such as CT scans or MRIs frequently appear normal in concussion cases, as concussions primarily involve functional rather than structural changes.

Recovery and Daily Functioning
Recovery experiences vary. Some individuals report resolution of symptoms within a short period, while others experience prolonged effects that influence daily routines.
During recovery, individuals may experience:
-
Reduced tolerance for cognitive or sensory stimulation
-
Difficulty performing tasks requiring sustained focus
-
Increased need for rest
-
Temporary limitations in work or daily activities
Medical management and recovery planning are typically guided by healthcare professionals based on symptom patterns and clinical evaluation.
Concussions and Insurance Claim Review
In insurance contexts, concussion-related claims are generally evaluated using medical documentation, diagnostic records, and treatment history. Because concussions do not produce visible injuries, often relies on medical documentation over time, clinical notes, and the incident description contained in available records.
Insurers typically review:
-
Initial medical assessments
-
Follow-up treatment records
-
Diagnostic findings
-
Documented functional limitations
The evaluation process varies by insurer, jurisdiction, and policy terms.
Complexity in Concussion-Related Claims
Some concussion claims resolve without complication, particularly when symptoms are short-lived. In other cases, prolonged recovery or overlapping injuries may introduce additional complexity into both medical management and claim review.
In more complex cases, readers often have additional questions about documentation, timelines, and administrative processes.

Final Thoughts
Concussions following car accidents are medically recognized injuries that may occur with or without direct head impact. Symptoms can present immediately or develop over time and may affect cognitive, physical, and emotional functioning.
Understanding how concussions occur, how they are evaluated, and how they are commonly reviewed in insurance settings can provide useful context for individuals navigating recovery after a collision. Medical evaluation and documentation play a central role in both health management and administrative review processes.
Last reviewed for informational accuracy: February 2026